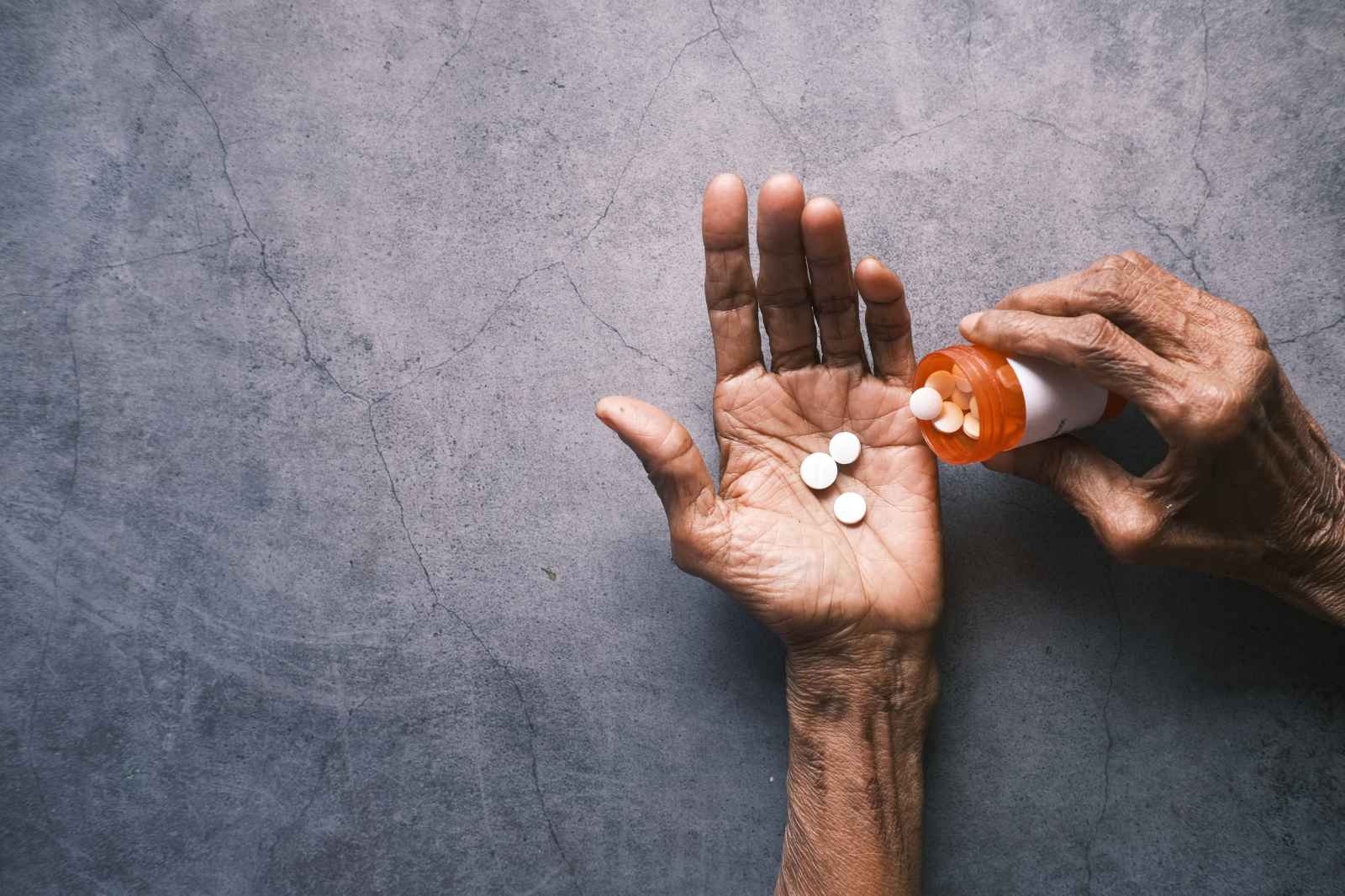
Type 2 diabetes is characterized by the body’s inability to produce or use insulin properly. Insulin is a hormone that acts like a key, “unlocking” cells to allow blood glucose to enter and provide the fuel your body needs to function. Glucose comes from the food we eat, and it’s produced in the liver. When the glucose in your blood can’t get into the cells, your blood sugar levels rise, causing major complications down the road.
The causes and risk factors for type 2 diabetes are wide-ranging, and addressing the underlying causes through lifestyle changes is the best way to manage your blood sugar and prevent complications of diabetes down the road. But lifestyle changes often aren’t enough to lower your blood sugar to healthy levels—especially when you’re first diagnosed. Medication is usually needed.
A range of medications are used to treat type 2 diabetes. Most of them lower your blood sugar levels in some way. Different medications have different mechanisms of action—some increase the production or activity of insulin in one way or another, while others perform a variety of actions to regulate the amount of sugar that moves into your bloodstream from the food you eat.
While diabetes medications can help prevent complications of diabetes and even improve heart or kidney function, they work best when combined with lifestyle changes that help you lower your blood sugar naturally, including eating a nutritious, low-carb diet and exercising regularly.
Here is a comprehensive run-down of the most common type 2 diabetes medications used today, along with how they work, who should take them, and what side effects you might expect from them.
Alpha-glucosidase inhibitors (Acarbose)
This class of drugs for type 2 diabetes is also sometimes used to treat people who have prediabetes to delay or prevent the onset of type 2 diabetes. The most commonly used AGI is acarbose, and it’s also the most widely studied one. Shown to increase life expectancy in people with type 2 diabetes. Other AGIs include miglitol and voglibose.
How do AGIs work?
AGIs inhibit carbohydrate absorption in the small intestine. They also inhibit enzymes that convert complex carbohydrates into simple ones.
AGIs are helpful for patients who have a high risk for hypoglycemia or lactic acidosis and can’t take diabetic drugs like metformin and sulfonylureas. AGIs have also been shown to reduce body weight. They’re useful for reducing postprandial hyperglycemia, since high blood sugar after a meal is associated with an increased risk for cardiovascular disease and other complications of diabetes, and they reduce glucose variability throughout the day. They don’t affect fasting insulin or serum triglyceride levels. AGIs are taken as a pill with the first bite of each meal.
Who shouldn’t take AGIs?
AGIs should be used with caution in children and in pregnant patients. AGIs aren’t as effective in people who eat a diet high in complex carbohydrates, and higher carb intake worsens potential gastrointestinal side effects. They shouldn’t be taken if you have a condition that causes excessive gas in the gut, those who have or are at risk for intestinal obstruction, or those with inflammatory bowel disease, colonic ulceration, or chronic intestinal disease.
What are the common side effects of AGIs?
The most common side effects of AGIs are gastrointestinal woes, including gas, diarrhea, and abdominal pain.
Biguanides (metformin)
Biguanides are a class of medication that lowers blood glucose levels. Metformin is the most commonly used drug in this class, and it’s used as a first-line treatment for type 2 diabetes. It can be taken on its own or in combination with other glucose-lowering drugs. Metformin is affordable, generally well-tolerated, and considered safe and effective for the vast majority of type 2 diabetes patients.
How does metformin work?
Metformin improves blood sugar control in a few ways. It inhibits the conversion of lactate and glycerol to glucose, which reduces the production of glucose in the liver. It also reduces the absorption of glucose from the intestines and even alters the gut biome, improving blood sugar stability. Metformin increases the uptake of glucose by the body’s tissues, and it’s also been found beneficial for reducing inflammation, cancer, and depression. Metformin is taken by pill typically twice a day .
Who shouldn’t take metformin?
Metformin is generally safe for most people with type 2 diabetes, but around five percent of those who start metformin therapy discontinue it due to severe gastrointestinal side effects, although it’s not clear why some people experience this. Researchers believe it may relate to metformin’s effect on the gut microbiome and are currently studying whether a person’s unique microbiome can influence the tolerance of this drug.
What are the common side effects of metformin?
The most common side effects of metformin are gastrointestinal-related and include nausea, abdominal discomfort, and diarrhea. The best way to reduce the risk of side effects is to take metformin with food. While metformin is not as significantly associated with lactic acidosis as other medications in the biguanide class, there’s a slight risk of this potentially fatal condition, but most research suggests that even in those with liver, kidney, or heart failure, lactic acidosis due to metformin is extremely rare.
Long-term Metformin use is associated with low vitamin B12 levels, which may have irreversible neurological effects, an increased risk of peripheral neuropathy. Your doctor will check your vitamin B12 levels and recommend an oral supplement if they’re too low.
Unlike other glucose-lowering medications, metformin rarely causes hypoglycemia, or low blood sugar.
DPP-4 inhibitors
Dipeptidyl peptidase 4 inhibitors are a blood sugar-lowering class of medications. Also known as gliptins, these drugs act on gut hormones that help stabilize blood sugar after eating food. DPP-4 inhibitors also have antihypertensive, anti-inflammatory, and antiapoptotic effects on the blood vessels, heart, and kidneys. These medications can be used alone or alongside other diabetes medications including metformin, sulfonylureas, thiazolidinediones, and insulin. DPP-4 inhibitors include:
- Alogliptin (alone or with metformin or pioglitazone)
- Linagliptin (alone or with metformin or empagliflozin)
- Saxagliptin (alone or with metformin)
- Sitagliptin (alone or with metformin or simvastatin)
How do DPP-4 inhibitors work?
DPP-4 is an enzyme that’s released within minutes of eating. It acts on certain hormones—most notably glucagon-like peptide-1 (GLP-1) and gastric inhibitory peptide (GIP)—that maintain stable glucose levels by increasing insulin secretion and reducing the secretion of glucagon. DPP-4 inhibitors immediately degrade DPP-4 enzymes, increasing GLP-1 and GIP levels and reducing post-meal and fasting blood sugar. These medications are taken as a pill once a day, before or after a meal.
Who shouldn’t take DPP-4 inhibitors?
People with type 1 diabetes or diabetic ketoacidosis shouldn’t take DPP-4 inhibitors. Some gliptins shouldn’t be taken by people who are sensitive to the drug or who have pancreatitis or a history of pancreatitis.
What are the common side effects of DPP-4 inhibitors?
The most common side effects of DPP-4 inhibitors sitagliptin and saxagliptin include upper respiratory tract infections, headache, and urinary tract infections. Sitagliptin, vildagliptin, and saxagliptin may be associated with pancreatitis. Although saxagliptin has been linked to a risk of heart failure, studies of gliptins didn’t show an increased risk for cardiovascular death, non-fatal stroke, or non-fatal myocardial infarction when compared with a placebo.
While gliptins have a low incidence of side effects, the risk of hypoglycemia increases with the addition of sulfonylureas to a DPP-4 inhibitor.
GLP-1 receptor agonists
Glucagon-like peptide-1 agonists are a class of medication that stimulates the production of insulin after a meal, delays gastric emptying, improves glucose uptake by the muscles, and slows the production of glucagon by the pancreas if your blood sugar levels are high. GLP-1 agonists have also been shown to promote weight loss, lower blood pressure and cholesterol, and reduce the risk for cardiovascular events. The most commonly prescribed GLP-1 agonists include:
- Albiglutide
- Dulaglutide
- Exenatide, injected twice-daily or once-weekly
- Liraglutide
- Lixisenatide
- Semaglutide
How do GLP-1 receptor agonists work?
Also known as incretin mimetics, GLP-1 receptor agonists copy (mimic) the action of the hormone GLP-1, which causes the pancreas to produce insulin after you eat. While the effects of the GLP-1 that’s produced by your body only last for a few minutes, GLP-1 receptor agonist medications last considerably longer, keeping your blood sugar levels stable and helping you feel fuller sooner. GLP-1 agonists are generally administered via injection, although the FDA recently approved an oral formulation of semaglutide.
Who shouldn’t take GLP-1 receptor agonists?
People who are pregnant and those with severe gastrointestinal diseases shouldn’t take GLP-1 agonists, and they’re not recommended for people who have a history of certain thyroid disorders. Tell your doctor if you have a history of pancreatitis or if you develop symptoms of pancreatitis while you’re taking a GLP-1 agonist.
What are the common side effects of GLP-1 receptor agonists?
The most common side effects of GLP-1 agonists include nausea, vomiting, headache, diarrhea, dizziness, and weakness. If you’re taking a sulfonylurea medication or long-acting insulin along with this medication, you may experience hypoglycemia. Knowing the symptoms of low blood sugar and how to treat it quickly is crucial if you’re taking this combination of drugs.
Meglitinides (repaglinide)
A class of antihyperglycemic medications prescribed to lower your blood sugar, meglitinides reduce blood glucose levels by stimulating the production of insulin in the body. It can be used alone—along with a healthy diet and regular exercise—or in combination with other blood glucose-lowering medications like metformin. However, it shouldn’t be taken with sulfonylureas.
Repaglinide is the most commonly used meglitinide, and it’s a safer treatment choice than metformin and sulfonylureas for people with chronic kidney disease or end-stage renal disease.
How does repaglinide work?
Repaglinide binds to beta cell receptors in the pancreas, stimulating the release of insulin. It’s absorbed rapidly by the body, and it has a short duration of action, which makes it ideal for helping to manage post-meal spikes in blood sugar. It’s taken around 30 minutes before each meal, up to three times per day.
Who shouldn’t take repaglinide?
Breastfeeding mothers, children under the age of 18, and people with severe liver dysfunction shouldn’t take repaglinide, and it should be used with caution in pregnant women. It’s not an effective treatment for people with type 1 diabetes or diabetic ketoacidosis.
What are the common side effects of repaglinide?
The most common side effects of repaglinide include hypoglycemia, weight gain, upper respiratory tract infections, and sinusitis. Hypoglycemia occurs more frequently with repaglinide when it’s combined with metformin, and when it’s used along with a thiazolidinedione, it may increase the risk for the swelling of the hands and feet. Less common side effects include diarrhea and joint pain. Repaglinide has a higher risk of cardiovascular events than metformin but a lower risk than sulfonylureas.
SGLT2 inhibitors
Sodium-glucose cotransporter-2 inhibitors are a class of medications prescribed along with lifestyle changes to lower blood sugar in people with type 2 diabetes. SGLT2 inhibitors lower hemoglobin A1C without increasing the risk for hypoglycemia, and they spur weight loss and improve cardiovascular and renal outcomes and mortality, especially for those who have heart failure or a history of cardiovascular events. SGLT2 inhibitors include:
- Canagliflozin (Invokana)
- Dapagliflozin (Farxiga)
- Empagliflozin (Jardiance)
How do SGLT2 inhibitors work?
SGLT2 inhibitors suppress the reabsorption of glucose in the kidneys, resulting in the excretion of excess sugar from the body through the urine. These medications are taken daily in pill form.
Who shouldn’t take SGLT2 inhibitors?
People who have renal insufficiency shouldn’t take SGLT2 inhibitors.
What are the common side effects of SGLT 2 inhibitors?
Although SGLT2 inhibitors are generally well-tolerated, side effects may include dehydration, genital yeast infections, and urinary tract infections. People who are taking SGLT2 inhibitors should be carefully monitored for euglycemic diabetic ketoacidosis, a rare but potentially life-threatening condition. Recent research shows that the SGLT2 inhibitor canagliflozin may increase the risk for bone fractures and lower-extremity amputation.
Sulfonylureas
The second most commonly prescribed type 2 diabetes medication after metformin, sulfonylureas are a class of medications that stimulate insulin secretion to lower blood sugar levels. Sulfonylureas are commonly used in people who can’t tolerate metformin, and they’re often prescribed in lower doses along with metformin. Glimepiride is the most commonly used sulfonylurea due to its relatively low risk for hypoglycemia. Other sulfonylureas include:
- Glyburide
- Tolazamide
- Tolbutamide
How do sulfonylureas work?
These medications work by stimulating the production of insulin in pancreatic beta cells regardless of blood sugar levels. They’re most effective for people who have had diabetes for less than five years, who are at a normal weight or overweight, and who have acceptable pancreatic function. Sulfonylureas are taken daily in pill form.
Who shouldn’t take sulfonylureas?
Elderly people, those with type 1 diabetes, and those who have had major surgery shouldn’t take sulfonylureas. You should also avoid these medications if you have a severe infection, malnutrition, or kidney or liver disease.
What are the common side effects of sulfonylureas?
Since sulfonylureas stimulate insulin secretion whether or not your blood sugar levels are high, taking this medication can cause hypoglycemia, especially after missing a meal, exercising, or taking high doses of sulfonylureas. If you’re taking this medication, know how to recognize symptoms of hypoglycemia and how to treat it quickly. Weight gain is also associated with sulfonylureas, so diet and exercise management is important while taking them.
Thiazolidinediones
Also called “glitazones,” thiazolidinediones (TZDs) are used alone or in combination with metformin or sulfonylureas to help manage type 2 diabetes. They’re also used to treat polycystic ovarian syndrome to help improve endothelial function and ovulation and reduce insulin resistance. Glitazones don’t cause hypoglycemia, and they can be taken by people who have renal diseases. The two medications in this class that are approved for use in the U.S. are:
- Rosiglitazone (alone or with glimepiride or metformin)
- Pioglitazone (alone or with alogliptin, glimepiride, or metformin)
How do thiazolidinediones work?
Thiazolidinediones regulate a wide range of metabolic pathways that ultimately increase insulin sensitivity in the body’s tissues and enhance the action of insulin. TZDs may also have anti-inflammatory and anti-cancer properties, and research shows beneficial effects for the heart. TZDs are generally taken once a day in pill form, with or without food.
Who shouldn’t take thiazolidinediones?
People who have heart failure shouldn’t take TZDs unless necessary, and then, only at the lowest possible dose, since they carry a risk of fluid retention and diastolic heart failure. Those with moderate to severe liver disease or dysfunction should take TZDs, nor should pregnant women, people with bladder cancer, or those who have a high risk of bone fractures.
What are the common side effects of thiazolidinediones?
TZDs are associated with a range of serious side effects, especially with long-term use. Your healthcare provider will help you weigh the benefits and risks of taking these medications, based on your personal medical history and risk factors. The most common adverse effects of TZDs include:
- Edema and congestive heart failure due to fluid retention
- Weight gain, especially with insulin use
- Increased risk of bone fractures
- Increased risk of bladder cancer
Insulin
When a combination of lifestyle changes and first-line medications aren’t enough to maintain healthy blood sugar levels, insulin therapy may be recommended for people with type 2 diabetes. Although insulin is most often associated with type 1 diabetes, it’s safe and effective for those with type 2 diabetes who need extra help managing blood sugar—it may be used to replace or complement existing medication. If insulin is an option your healthcare team is considering, you’ll receive all of the information and education you need to make insulin therapy an easy, unobtrusive treatment that’ll keep you healthy and active for the long-term.
Forward helps you manage your type 2 diabetes
As your primary care provider, Forward helps you keep your blood sugar under control for long-term good health. Your Forward physician and care team will work with you to develop just the right lifestyle, medication, and monitoring plan to manage your blood sugar for the long-term. Forward physicians stay on top of new and emerging research to provide you with the best treatment options for you. Through a variety of resources, management strategies, and programs, we’ll help you set and achieve health goals, including losing weight, maintaining healthy blood glucose levels, and even reversing your type 2 diabetes.